Table of Contents
Where we are, and how we got here
by Colby Joyner
Before we begin, I should give full disclosure. I write prescriptions for opioids. I write them often, and I work in chronic pain management. If anyone states this would make me unabashedly pro-opioid as a chronic pain medication, let me first say that further regulation and reduction of prescriptions would actually make my job easier. As it currently stands, opioids have no maximum dose nor rate of dose escalation, just a heavily-implied assumption of risk as the dose goes up. If a law is passed tomorrow that gives clear limits to doses and dose increases, my job, though forced, becomes multi-fold easier. The guesswork would be eliminated.
However, the subjectivity of pain, range of severity across the multitude of chronic pain conditions, and variance of medication efficacy from patient to patient complicate management and the “appropriate” dose to control both pain and risk, which makes the construction of such legislature difficult. As a result, a huge amount of intellectual concentration is focused on each patient as an individual, which is the real challenge in pain management. If that challenge were taken away, I would have a simpler workday, but it does not guarantee better patient care, neither does it change the facts of this article and how we should responsibly approach the problem as a whole.
 A young man is doing something he has done many times before. Of course, he’s been using for years. This time, though, he’s playing it “safe.” He knows there are risks. He has friends who have died recently from heroin that was mixed with more powerful drugs. He decides to take less than he usually does. He grabs his burnt spoon, heats the water and powder mixture by the flame of a lighter, and injects it into his bloodstream. It feels like what he wanted, the incredibly short high and feeling of euphoria that can last as short as forty-five seconds with peak effects that last less than a few hours. He used to spend days chasing those forty-five seconds. However, it does not ease off this time. Within minutes the driving force behind the respiratory system in his brain is struck down by a flood of opiate molecules. He stops breathing. He dies.
A young man is doing something he has done many times before. Of course, he’s been using for years. This time, though, he’s playing it “safe.” He knows there are risks. He has friends who have died recently from heroin that was mixed with more powerful drugs. He decides to take less than he usually does. He grabs his burnt spoon, heats the water and powder mixture by the flame of a lighter, and injects it into his bloodstream. It feels like what he wanted, the incredibly short high and feeling of euphoria that can last as short as forty-five seconds with peak effects that last less than a few hours. He used to spend days chasing those forty-five seconds. However, it does not ease off this time. Within minutes the driving force behind the respiratory system in his brain is struck down by a flood of opiate molecules. He stops breathing. He dies.
He becomes a statistic added to the mounting evidence against opiate use — another increase to the number that has been used to encourage empathy and incite social activism. The tale of patients coming from far and wide without as much as a cough were offered extremely high doses of pain medicine every month without any physical examination. Got the cash? You got the script. That was at least the external perception of many chronic pain institutions that offer opioids—the pill mills. Their plight perpetuates the constant, inevitable link between illicit drug users and chronic pain patients.
Did the Chronic Pain Pill Mills Do It?
There is strong evidence that prescriptions were declining well before this year. The Center for Disease Control’s (CDC) own data showed a decrease of 18 percent in opioid prescriptions in 2015 compared to 2010, before this surge of public awareness and more drastic changes, including a decline over that five-year period in three-fourths of counties nationwide. Providers are writing significantly less prescriptions than 2010 and we are having more than double the overdose deaths [1,2]. That is the single most-compelling piece of evidence I have found that suggests today’s prescriptions are not the culprit for the recent death rise. Naysayers will quickly point out that opioid prescriptions are still triple 1999 levels, but the kind of precipitous rise from 1999 to 2010 does not explain the figures of the last few years. In fact, the largest jumps in death rate after 2005 have occurred in 2015 and beyond despite declining prescriptions being written. Something else has changed.
 The most commonly used statistic, and therefore the most vital driver of legislative and regulatory change, includes all opioid-related deaths without differentiation between the substances involved. This includes our young man from the opening paragraph. This also includes a young adult who mixes pain pills, sedatives, cocaine and alcohol in the same night resulting in his death. Likewise, it includes a chronic pain patient who overdoses on his oxycontin accidentally. The key difference is that there is a huge discrepancy in relative risk for an active intravenous drug user, a recreational mixer of substances they are never prescribed, and someone only taking prescription medications. In the studies cited by the CDC guidelines for opioid prescribing for chronic pain in the primary care setting –they found that death from prescription opioids was dose-dependent—higher dose means higher risk.
The most commonly used statistic, and therefore the most vital driver of legislative and regulatory change, includes all opioid-related deaths without differentiation between the substances involved. This includes our young man from the opening paragraph. This also includes a young adult who mixes pain pills, sedatives, cocaine and alcohol in the same night resulting in his death. Likewise, it includes a chronic pain patient who overdoses on his oxycontin accidentally. The key difference is that there is a huge discrepancy in relative risk for an active intravenous drug user, a recreational mixer of substances they are never prescribed, and someone only taking prescription medications. In the studies cited by the CDC guidelines for opioid prescribing for chronic pain in the primary care setting –they found that death from prescription opioids was dose-dependent—higher dose means higher risk.
The CDC combined data from four studies of non-cancer chronic pain patients and found the risk of the highest dose group for fatal overdose was 0.25 percent, or 1-in-400 patients over a period of up to 13 years [3]. This group was taking the equivalent dose, regardless of medicine, of at least 100 milligrams of morphine daily. So, the group with the highest risk for fatal overdose, receiving the most medication that was measured, had a 1-in-400 chance of dying due to opioids in over a decade. A death rate of near 0.25 percent over this period is still too high in a general sense, and many of these patients most likely had glaring warning signs of noncompliance before these overdoses. But, if this is the risk of only the riskiest chronic pain patients, it will not yield an epidemic anywhere near the scale that we are experiencing today [4]. In other words, chronic pain patient deaths cannot be blamed for it.
 A study of over 130,000 opioid overdose patients throughout 2010 that were treated in the emergency room showed that only 13 percent had chronic pain conditions [5]. The chronic pain patients aside, there is still an argument that the pain prescriptions are to blame. This is because of evidence that most street drug users start with prescription drugs, of which they are most likely to buy or get from family [6]. Are these pills out in the wild from pill mills masquerading as pain management? From 2007-2010 primary care wrote nearly half of all opioid prescriptions [7]. In 2014, 65 percent of opiate prescriptions were for short-term use (3 weeks or less). This means about 1/3 of prescriptions were for chronic pain. These are the patients that are followed monthly and often subject to a pain contract, regular urine drug tests, and random pill counts to ensure they have the right amount of medication [8]. Those receiving scripts for acute pain are subject to none of these measures nor held accountable for what may or may not be in their system.
A study of over 130,000 opioid overdose patients throughout 2010 that were treated in the emergency room showed that only 13 percent had chronic pain conditions [5]. The chronic pain patients aside, there is still an argument that the pain prescriptions are to blame. This is because of evidence that most street drug users start with prescription drugs, of which they are most likely to buy or get from family [6]. Are these pills out in the wild from pill mills masquerading as pain management? From 2007-2010 primary care wrote nearly half of all opioid prescriptions [7]. In 2014, 65 percent of opiate prescriptions were for short-term use (3 weeks or less). This means about 1/3 of prescriptions were for chronic pain. These are the patients that are followed monthly and often subject to a pain contract, regular urine drug tests, and random pill counts to ensure they have the right amount of medication [8]. Those receiving scripts for acute pain are subject to none of these measures nor held accountable for what may or may not be in their system.
Opioids for acute pain also has a much more important faction: inclusion criteria. A proper chronic pain patient requires a history that backs up their chronic pain story. They often have multiple surgeries, years of doctor’s visits, and a history of compliance or noncompliance with pain medication. Acute pain sufferers need only a condition that might have pain right now. A broken bone, pulled tooth, or a common rotator cuff tear can lead to an opiate prescription. The use in these patients might be more troubling since they have no guarantee of future prescriptions. They do not have diagnoses that warrant considering long-term narcotic use. This means if you get hooked, illicit use is your only option.
Starting Young
Patient age is also likely to be lower in acute pain, with prescriptions also being written for adolescents and teenagers. In 2011, Columbia University’s National Center on Addiction and Substance Abuse found that 90 percent of Americans who suffered from addiction started abusing substances before age 18. Furthermore, they found that 25 percent who simply began any sort of use of addictive substances before age 18 became addicted later on, versus 4 percent who started at age 21 or older. This monstrous discrepancy suggests that we should heed more caution before starting any addictive substance in youth, including stimulants for ADD, tranquilizers for anxiety, or narcotics for pain relief. However, one-third of 12th graders entering the University of Michigan in 2010 that admitted using a prescription narcotic in the last year stated they got it from a prescription [9].
 Data on addiction repeatedly suggests it results from having a certain combination of personality and genetics that makes one more susceptible to addiction. It is difficult to ascertain if adding addictive substances changes this biochemistry or simply unlocks it. A relatively low percentage of opioid users become addicted, but when they do, it is often accompanied by abuse of other substances. A good chronic pain clinic can identify this.
Data on addiction repeatedly suggests it results from having a certain combination of personality and genetics that makes one more susceptible to addiction. It is difficult to ascertain if adding addictive substances changes this biochemistry or simply unlocks it. A relatively low percentage of opioid users become addicted, but when they do, it is often accompanied by abuse of other substances. A good chronic pain clinic can identify this.
Begin the Crackdown
With no data readily available to determine the source of the increase in overdoses, the most obvious and easiest maneuver available to legislatures was to control prescriptions. And they did. The federal and state governments have taken large, sweeping moves against over-prescribing of pain-killers and mitigation of their risk. These include the March 2017 CDC guidelines against higher doses being managed by primary care, the FDA request that the extended release version of brand-name oxymorphone, Opana ER, be removed from the market, and many states limiting prescriptions for acute pain among other measures.
However, despite the efforts and resulting responses, death rates continue to rise. Because death rates take an exceedingly long amount of time to certify, up-to-date data is difficult to find nationally, but is more readily available at the state and county levels. The New York Times found that 2016 drug overdose deaths are likely to exceed 60,000 people at a rate that is growing in a near-exponential pattern with no signs of slowing down. Data from 2017 is even harder to gather, but the Times projects a momentous rise in deaths in six Ohio counties, even compared to 2016. The same model projects the 2017 numbers to more than quadruple the numbers from 2010 [10]. We must not be seeing the fruits of our labor yet. It’s too early. If we double down on limiting these obviously over-prescribed drugs, things will turn around. Right?
 We have accomplished the task by limiting and stigmatizing the users and prescribers of prescription opioids at a staggering pace. In my practice, we are seeing patients being referred for pain management faster than ever—two weeks after surgery or days after receiving an MRI confirming the severe degenerative condition of their back and a letter saying that no further surgery is recommended, implying pain management or bust. Acts such as the CDC guidelines have had a profound effect on primary care providers, causing many to cease writing prescriptions all-together in fear of action against them by the Drug Enforcement Agency (DEA) or their state medical board. Many of our patients have arrived at our doors with a more troubling story: “My doctor won’t write this anymore.” “My dose was cut in half, and he told me to find somewhere else after being there for years.” Their records back this story of rapid reduction. I will refrain from telling how inhumane such a rapid reduction of medicine and then abrupt discharge is, particularly after years of a mutually complicit medical provider giving them a monthly prescription, but it is a testament to how effective actions like the CDC guidelines have been at changing provider habits.
We have accomplished the task by limiting and stigmatizing the users and prescribers of prescription opioids at a staggering pace. In my practice, we are seeing patients being referred for pain management faster than ever—two weeks after surgery or days after receiving an MRI confirming the severe degenerative condition of their back and a letter saying that no further surgery is recommended, implying pain management or bust. Acts such as the CDC guidelines have had a profound effect on primary care providers, causing many to cease writing prescriptions all-together in fear of action against them by the Drug Enforcement Agency (DEA) or their state medical board. Many of our patients have arrived at our doors with a more troubling story: “My doctor won’t write this anymore.” “My dose was cut in half, and he told me to find somewhere else after being there for years.” Their records back this story of rapid reduction. I will refrain from telling how inhumane such a rapid reduction of medicine and then abrupt discharge is, particularly after years of a mutually complicit medical provider giving them a monthly prescription, but it is a testament to how effective actions like the CDC guidelines have been at changing provider habits.
The guidelines, however, are just that. They have no hard limits. There is no legal action implicit for breaching them. Regardless, providers not specializing in pain management are still leaving opioid management in its entirety at an alarming rate, causing these patients to take one of three paths: find another provider, endure the intense withdrawals and rebound pain that can occur from abruptly stopping the medicine after years of use, or run to the streets and take what is available. The problem is that there is not always another provider, and even on the streets, the pain pills are not always an option.
 What changed?
What changed?
Street opioids changed. Their users have changed as well. Heroin abuse has shifted from low-income minorities to affluent Caucasian populations. No population has seen a higher rise than the young adult white female. White populations overall have seen a six-fold increase in ten years. Populations that have low susceptibility to any hard drugs suddenly started having a rise in use. Overdose death data also shows that though the average age of use has increased over the years, the average age of overdose death has become bimodal and significantly younger on average [11, 12]. This has created a system shock not only with the risks involved, but because these populations are not used to these risks. Alcohol and marijuana, sure, but heroin?
Heroin is relatively well-known. It can be taken orally, snorted (sniffed into the nasal passage), or, most dangerously, injected intravenously. It produces a high that is relatively short-lived and thus has to be dosed relatively often. It is a downer, which means its effects of withdrawals are generally worse than uppers like cocaine. It has also been around for a long time. The effects responsible for its rise are simple economics, namely cost and availability. Potent heroin has become more widely available and cheaper [13]. The Washington Post may have said it best with the title of their 2015 article, “Why a bag of heroin costs less than a pack of cigarettes,” which described how the knowledge of the increasing price of street prescription opiates motivated Mexican drug cartels to increase production and move it to more parts of the country [14]. That may explain the increase in use, but not necessarily deaths. Heroin users, though they certainly had a lower life expectancy than most, historically could use for decades without a fatal overdose.
Enter fentanyl. Some may recognize fentanyl as its historical form of a skin patch, used to help chronic pain suffers for three days at a time. Though the patch has the same molecules as the fentanyl on the street and is also wildly dangerous when abused, it has also been around for a long time without causing this level of crisis. The problem now is bulk fentanyl powder funneled from Mexico and domestically made in labs. If a cartel is moving heroin now, they have to beat the competition’s heroin. It is doing to heroin what heroin did to the street prescription drugs: be cheaper, stronger, and more available.
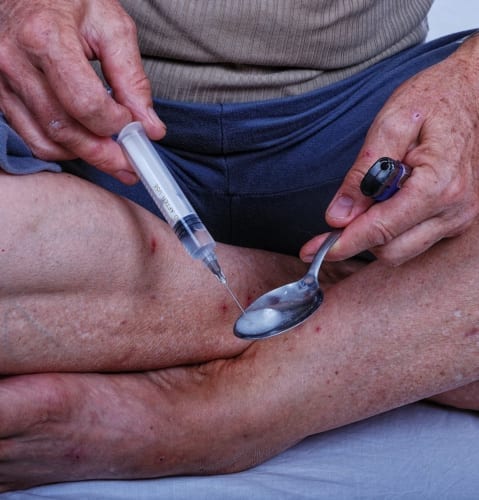 Fentanyl is up to one-hundred times more potent than morphine and fifty-times stronger than heroin [15, 16]. A quick internet search for the lethal dose of fentanyl versus heroin will lead to a troubling image where a seemingly insignificant amount of white powder, not much more than the amount of salt you would see on a couple of french fries—an amount that would only cover about the size of Abraham Lincoln’s face on a penny. The lethal dose of heroin looks like a mountain in comparison. Drug dealers are using this cheaper, stronger alternative to improve profit margins at the expense of their users’ lives. When mixed, heroin and fentanyl are indistinguishable. As one of my dependency patients said, “It’s impossible to play it safe anymore.” A heroin user may have friends who have died and resist for as long as possible, but end up using again. They may only shoot up half or a quarter what they usually do, but if the heroin is cut with enough fentanyl, it does not matter. That person will still overdose. If that was not troubling enough, there are parts of the country where it is extremely difficult to find heroin that does not also contain fentanyl [17].
Fentanyl is up to one-hundred times more potent than morphine and fifty-times stronger than heroin [15, 16]. A quick internet search for the lethal dose of fentanyl versus heroin will lead to a troubling image where a seemingly insignificant amount of white powder, not much more than the amount of salt you would see on a couple of french fries—an amount that would only cover about the size of Abraham Lincoln’s face on a penny. The lethal dose of heroin looks like a mountain in comparison. Drug dealers are using this cheaper, stronger alternative to improve profit margins at the expense of their users’ lives. When mixed, heroin and fentanyl are indistinguishable. As one of my dependency patients said, “It’s impossible to play it safe anymore.” A heroin user may have friends who have died and resist for as long as possible, but end up using again. They may only shoot up half or a quarter what they usually do, but if the heroin is cut with enough fentanyl, it does not matter. That person will still overdose. If that was not troubling enough, there are parts of the country where it is extremely difficult to find heroin that does not also contain fentanyl [17].
Even more disturbing is the animal anesthetic for large animals (such as elephants) carfentanil, now also in the drug supply. This form of fentanyl is so potent an amount the size of a salt grain can kill, ten-thousand times stronger than morphine. First-responders may be recommended to wear gloves when arriving at scenes of suspected opioid overdose, and a child in Miami died from fentanyl skin contact in June [18, 19]. In a three-week period last summer, the DEA found eight of 208 overdoses to show carfentanil in Cincinnati [20].
 How far-reaching has this shift in drug composition been? Since 2011, fatal overdoses of prescription opioids have stopped rising, coinciding with the reduction of prescriptions being written [15]. Massachusetts found the presence of prescription opioids decrease from about a quarter of overdoses in 2014 to less than a tenth in the fourth-quarter of 2016 [21]. Meanwhile, overdoses with one or both of heroin and fentanyl now make up over half of deaths in the USA. In British Columbia, Canada, Fentanyl is in 72 percent of overdose deaths this year, up from 25 percent in 2014 [22]. The discrepancy may be even wider than it appears, given that the prescription opioids are reported in overdoses that “involve” them. This can mean the person overdosed on heroin and fentanyl, but happened to have a prescription drug on board as well. This certainly would make their condition worse, but heroin and fentanyl are still the predominant reason for death. In short, it has been catastrophic.
How far-reaching has this shift in drug composition been? Since 2011, fatal overdoses of prescription opioids have stopped rising, coinciding with the reduction of prescriptions being written [15]. Massachusetts found the presence of prescription opioids decrease from about a quarter of overdoses in 2014 to less than a tenth in the fourth-quarter of 2016 [21]. Meanwhile, overdoses with one or both of heroin and fentanyl now make up over half of deaths in the USA. In British Columbia, Canada, Fentanyl is in 72 percent of overdose deaths this year, up from 25 percent in 2014 [22]. The discrepancy may be even wider than it appears, given that the prescription opioids are reported in overdoses that “involve” them. This can mean the person overdosed on heroin and fentanyl, but happened to have a prescription drug on board as well. This certainly would make their condition worse, but heroin and fentanyl are still the predominant reason for death. In short, it has been catastrophic.
But Does A Really Lead to B?
You may have noticed a common line between chronic pain patients and illicit opioid users. The reduction in the amount of pain prescriptions and providers writing them has led to the detriment of both populations. Let me explain.
Chronic pain patients are facing difficulty finding providers who will treat them. They are often unwanted at pharmacies, regardless of how high their dose may be. They went to a provider at least twelve times every year, and some of them have done this for decades. Then, with a loss of a provider, they face a choice. Many will responsibly taper and learn to tolerate their pain or find another provider. Some will find the withdrawals and pain too much to bear and seek another path. Remember when I said pain pills on the streets might not be an option?
 Following supply and demand, the decrease in prescriptions on the street, both from a decrease in prescriptions and tighter measures to ensure compliance among patients, has resulted in the street-cost of prescription drugs to increase significantly. This, along with the decreased price and increased availability of heroin and fentanyl has pushed others into hard drug use much faster than they would have otherwise. The National Survey on Drug Use and Health suggests that non-medical use of prescription opioids peaked in 2012 and is now under 2002 levels, though that is nothing to be proud of if a large portion of those former users are now on harder drugs [23].
Following supply and demand, the decrease in prescriptions on the street, both from a decrease in prescriptions and tighter measures to ensure compliance among patients, has resulted in the street-cost of prescription drugs to increase significantly. This, along with the decreased price and increased availability of heroin and fentanyl has pushed others into hard drug use much faster than they would have otherwise. The National Survey on Drug Use and Health suggests that non-medical use of prescription opioids peaked in 2012 and is now under 2002 levels, though that is nothing to be proud of if a large portion of those former users are now on harder drugs [23].
For those who want to only use heroin as a last option, even taking the drugs they believe to be prescription painkillers may not be possible. An increase in fake pills filled with, you guessed it, heroin and fentanyl made to look like oxycodone and other traditional pills has begun, and in some places, become dominant. A special agent in charge of the DEA’s New England division even said that if you are buying prescription pain pills on the street, they are probably fakes [24]. To make things worse, just like how the strength of heroin and fentanyl makes them much deadlier, a patient may find themselves overdosing on a couple of fake pills that had enough fentanyl when it normally would take a dozen to get the same response. Since pills have an even greater profit margin, often reaching $30 or more per pill, this sort of behavior will continue to rise when $1 of bulk fentanyl can turn into $1,000 in fake pills on the streets.
To be clear, the goal is not having more prescription painkillers on the streets. However, it is undeniable that recreational use of prescription drugs is less lethal than heroin and fentanyl. If we are going to restrict one side, we must provide proper support so to avoid people from moving to a riskier alternative. We want to avoid people moving from A to B, where A is a user of prescriptions painkillers and B is much worse, a user of heroin and fentanyl. Up until this point, we have been using laws, regulations, and actions by agencies to do our best to restrict people from becoming A, believing that it will then stop B from growing. But, what if you are an A that will never become a B, or, even worse still, already a B? If that is the case, what we have done will do little to help you. Those who are already a B will continue to die. The As who would never be Bs are inconvenienced, mistreated, and actually given a larger risk of becoming Bs. Those who become Bs and skip being an A altogether are not helped. Those benefitting are future abusers of prescription opiates. The ones driving up the death rates, current heroin users, do not benefit from prescription opioid restriction. We are inadvertently sacrificing two populations: isolated chronic pain patients and the heroin users unaffected by further prescription control.

What to do about it
Instead of continued prescription control, efforts should be focused on the population who is overdosing at the highest rate. Unfortunately, the public is largely unaware of the most effective standards of treatment. Awareness of naloxone, particularly its nasal spray version Narcan, has increased due to it being carried by law enforcement and first responders. New initiatives have focused heavily on this medication due to its ability to give back a life in an instant. Cincinnati’s Hamilton County recently revealed a plan to quadruple the distribution of the drug. However, in this form, naloxone will only stop an overdose in progress, but not discourage heroin use itself–much like how an Epi-pen may save someone allergic to bee stings, but does not keep them from walking through the bees. Furthermore, if you gave every heroin user ten doses, the same number of overdoses would happen, there would simply be the chance of less lethal overdoses.
Opioid overdoses also require someone else to do the dosing, when many overdose victims are found alone. Some enforcement groups are also worried that naloxone is seen as a “get out of jail free” card that allows users to continue reckless use without fear of overdose [25]. Relying on this as a failsafe is also straining economically. Middletown, Ohio, a town of less than 50,000 people, is on pace to spend more than $100,000 on Narcan this year [26]. A councilman even suggested limiting overdose EMS response to no more than two per person [27]. Third overdose? No response. A treatment that often requires an emergency response and tiptoeing the line of life and death cannot be a foundational treatment.
Fortunately, patients tend to do exceedingly-well with medication-assisted treatment itself, but has its own challenges. Detox centers are often highly expensive and have poor long-term results without being coupled to counseling and medication therapy [28]. Methadone requires high doses (commonly higher than severe chronic pain doses), is itself significantly susceptible to overdoses, and is described as one of the hardest opioids to taper over time, feeding the “you are just trading one drug for another” argument. Methadone treatment also requires going to a specialized methadone clinic that often requires daily visits, meaning that if heroin already didn’t put a stop to living a normal life, quitting heroin using these methods most certainly will [29].
 The opioid buprenorphine is a more favorable alternative when packaged with naloxone (the same drug in the aforementioned Narcan). Available in sublingual films (Suboxone) and tablets (Zubsolv, generics), the medication can be dosed once daily and patients are monitored on a monthly basis, allowing for a much more sustainable and “normal” lifestyle. Buprenorphine may also be the safest widely-available opioid [30]. It is extraordinarily difficult to find good records of a couple of cases, much less many cases, of adults overdosing on buprenorphine by itself. The data you can readily find cites other substances also being used [31]. Buprenorphine is sometimes used by heroin addicts as a bridge between doses, controlling their withdrawals. Because of this, it is sometimes misunderstood as a more dangerous medication than is warranted. The DEA backs up this by scheduling buprenorphine as a schedule III medication, warranting less control and caution than the schedule II substances that include all traditional opioids and methadone (lower schedule number means more controlled). However, buprenorphine treatment can be expensive, particularly in comparison to methadone, due to the lack of low-cost generic options.
The opioid buprenorphine is a more favorable alternative when packaged with naloxone (the same drug in the aforementioned Narcan). Available in sublingual films (Suboxone) and tablets (Zubsolv, generics), the medication can be dosed once daily and patients are monitored on a monthly basis, allowing for a much more sustainable and “normal” lifestyle. Buprenorphine may also be the safest widely-available opioid [30]. It is extraordinarily difficult to find good records of a couple of cases, much less many cases, of adults overdosing on buprenorphine by itself. The data you can readily find cites other substances also being used [31]. Buprenorphine is sometimes used by heroin addicts as a bridge between doses, controlling their withdrawals. Because of this, it is sometimes misunderstood as a more dangerous medication than is warranted. The DEA backs up this by scheduling buprenorphine as a schedule III medication, warranting less control and caution than the schedule II substances that include all traditional opioids and methadone (lower schedule number means more controlled). However, buprenorphine treatment can be expensive, particularly in comparison to methadone, due to the lack of low-cost generic options.
Regardless of the choice between methadone and buprenorphine, the return on investment of these treatments, in conjunction with counseling, would be far more effective than simply increasing Narcan availability. These methods have the potential of ceasing the heroin use entirely, reducing the chance of exposure to other drugs like fentanyl, and allowing for the type of interruption necessary to break such a life-consuming habit. We have to make receiving this treatment easier than continuing to use heroin. It would be a focused effort in death reduction and life change without the unintended consequence of damaging legitimate users of opioid medications.
Dealing with opioid addiction and responsible prescribing is nuanced. It is a complex matter that requires the consideration of many factors and the ability to avoid thinking in absolutes. It requires weighing current and future misuse while humanely treating those who have relied on these medications for years. For these humans, lives are destroyed before the first moment of overdose. Likewise, they can be saved after it — but we would do better if we never had to in the first place.
References:
- https://www.huffingtonpost.com/entry/new-numbers-reveal-huge-disparities-in-opioid-prescribing_us_5991a8c4e4b0caa1687a61e6
- https://www.cdc.gov/media/modules/dpk/2016/dpk-pod/rr6501e1er-ebook.pdf
- https://www.vox.com/science-and-health/2017/8/1/15746780/opioid-epidemic-end
- https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/1918924
- https://www.drugabuse.gov/publications/research-reports/relationship-between-prescription-drug-heroin-abuse/prescription-opioid-use-risk-factor-heroin-use
- https://www.ncbi.nlm.nih.gov/pubmed/25896191
- https://www.nejm.org/doi/pdf/10.1056/NEJMra1507771
- https://www.drugabuse.gov/
- https://www.nytimes.com/interactive/2017/06/05/upshot/opioid-epidemic-drug-overdose-deaths-are-rising-faster-than-ever.html
- https://www.theguardian.com/society/2017/mar/29/us-heroin-use-has-increased-almost-fivefold-in-a-decade-study-shows
- https://jamanetwork.com/journals/jamapsychiatry/fullarticle/1874575
- https://www.drugabuse.gov/publications/research-reports/relationship-between-prescription-drug-abuse-heroin-use/heroin-use-driven-by-its-low-cost-high-availability
- https://www.washingtonpost.com/news/to-your-health/wp/2015/08/27/why-a-bag-of-heroin-costs-less-than-a-pack-of-cigarettes-2/
- https://www.nytimes.com/interactive/2017/08/03/upshot/opioid-drug-overdose-epidemic.html?smid=fb-nytimes&smtyp=cur
- https://www.cdc.gov/
- https://www.huffingtonpost.com/entry/drug-war-no-heroin-without-fentanyl_us_59a6f72de4b063ae34daa40f
- https://www.cnn.com/2017/07/19/health/miami-boy-overdose-fentanyl-bn/index.html
- https://time.com/
- https://time.com/4485792/heroin-carfentanil-drugs-ohio/
- https://globalnews.ca/news/3637148/fentanyl-overdoses-canada-2017/
- https://www.latimes.com/opinion/op-ed/la-oe-hari-prescription-drug-crisis-cause-20170112-story.html
- https://www.tennessean.com/story/news/investigations/2017/03/26/paramedics-opioid-crisis-overdose-antidote-mixed-blessing/98544310/
- https://www.cincinnati.com/story/news/2017/09/07/hamilton-county-boost-narcan-400-percent-fight-overdose-deaths/624288001/
- https://www.usatoday.com/story/news/nation/2017/06/28/ohio-councilman-suggests-three-strikes-law-halt-overdose-rescues/434920001/#
- https://lacrossetribune.com/news/high-cost-of-opioid-crisis-unbearable/article_fceb4db3-275a-50c8-a707-82d2cc77152a.html
- https://www.cochrane.org/CD002209/ADDICTN_methadone-maintenance-therapy-versus-no-opioid-replacement-therapy
- https://bmjopen.bmj.com/content/5/5/e007629
- https://www.ncbi.nlm.nih.gov/pubmed/26305073
Author

Colby Joyner is a graduate of Wingate University with a Master’s degree, Physician’s Assistant. He works with patients to minimize pain, improve function, and increase their quality of life.
Further Reading
- WBIR – School system to hold education forums on opioid threat
- WTOP – Educators get more involved fighting Maryland opioid crisis
- Click Orlando – Central Florida schools respond to opioid crisis
